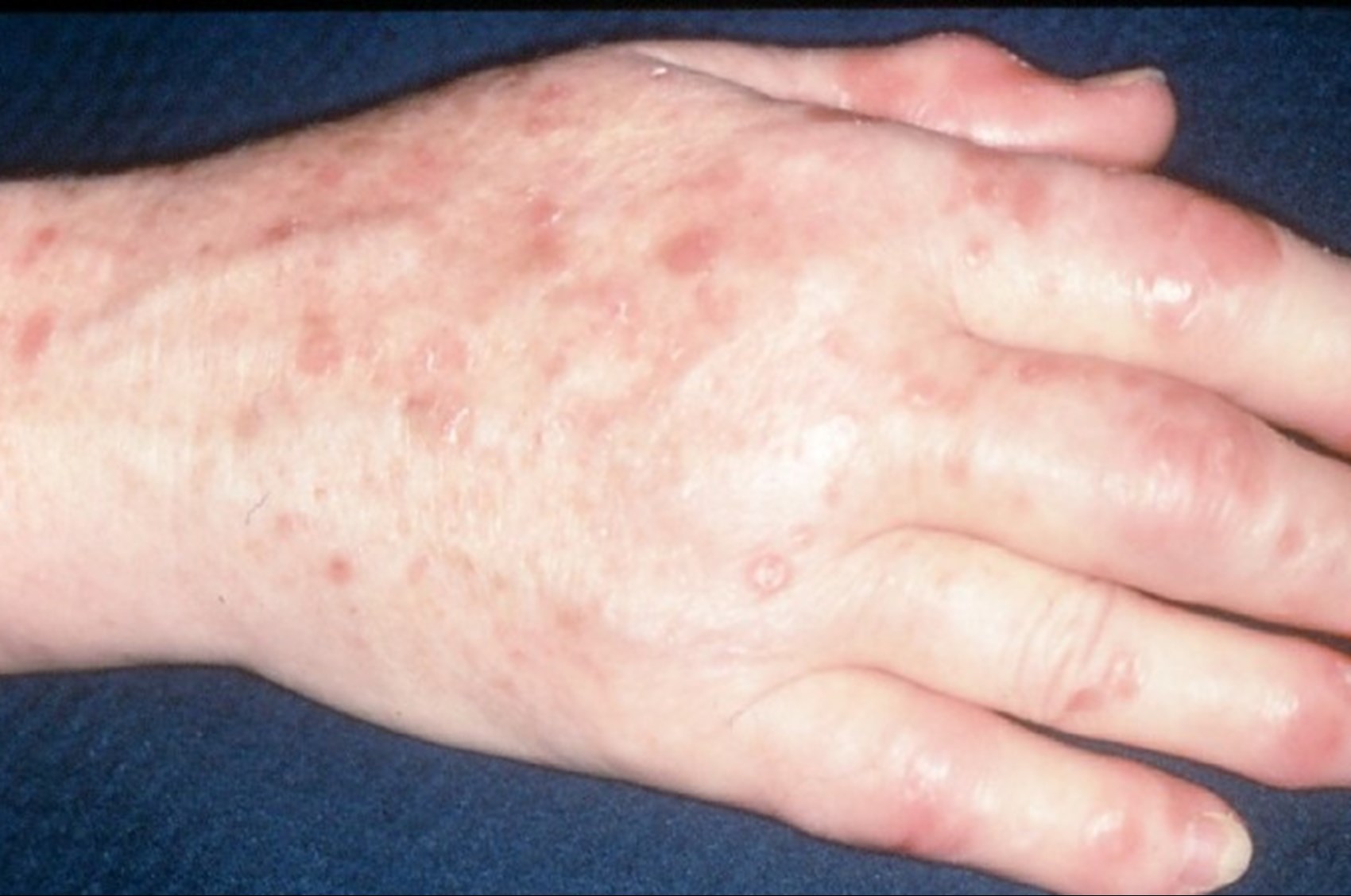
What happens in psoriatic arthritis?
Psoriatic arthritis (PsA) is a form of arthritis affecting individuals with psoriasis.
- Psoriatic arthritis (PsA) is a form of arthritis affecting individuals with psoriasis.
- Joints become inflamed, which causes pain, swelling and stiffness.
- Tendons may also become inflamed and cause pain (often around the heel or in the elbow).
- Joints are typically stiff after resting, particularly early in the morning or in the evening.
- Around 1 in 4 (25%) of those with psoriasis may develop some form of arthritis.
- In around 8 out of 10 (80%) the arthritis develops after the appearance of psoriasis.
- Some people may develop a condition of the eye (uveitis) which may cause redness and inflammation. If you are concerned about this, seek medical advice.
- People with psoriatic arthritis often report feeling fatigued or exhausted.
- There is some evidence that people with psoriasis and/or psoriatic arthritis might have a slightly increased cardiovascular risk (heart disease). See Psoriasis and the heart
How do joints and tendons become inflamed?
The function of a joint is to allow movement to occur between bones. In the joint, the end of the bone is covered with cartilage, around which is a capsule lined by a membrane called synovium.
This membrane makes the fluid that lubricates the joint space, allowing movement. In arthritis the synovial membrane becomes inflamed and releases substances that cause inflammation.
The inflamed synovium releases more fluid than normal and so the joint becomes tender and swollen. Persistent inflammation may lead to damage to the cartilage and erosion of the underlying bone.
The synovial membrane also lines and lubricates tendons, so overproduction of synovial fluid can also cause tendon inflammation.
What is different about psoriatic arthritis?
There are several features that distinguish psoriatic arthritis from other forms of arthritis.
- The pattern of joints that may be involved is different.
- Psoriatic arthritis may just affect a small number of joints (oligoarthritis) or many joints (polyarthritis).
- Most commonly the psoriatic arthritis is asymmetric in pattern (unlike rheumatoid arthritis, which is symmetrical).
- Psoriatic arthritis may affect the end joints of fingers, often corresponding with the fingers that have psoriatic nail involvement. See Nail Psoriasis
- When psoriatic arthritis affects the joints of the spine and sacroiliac joints it is called spondylitis (similar to ankylosing spondylitis). This can result in stiffness and pain of the back or neck.
- An entire toe or finger can become swollen or inflamed so called ‘sausage finger‘ (dactylitis).
- Some people have involvement of the jaw (temporomandibular joint – TMJ), where pain occurs on one or both sides of the face near the ear.
- Joints affecting the rib cage, particularly where they meet the sternum or breastbone.
- Psoriatic arthritis may affect where the tendons connect to the bone (enthesitis). Common areas to be affected include the heel and ankle.
- Psoriatic arthritis may cause joints to become stiff and limit their range of movement. In some severe cases the joint may fuse, with the result that it cannot be moved.
- Importantly, the absence of rheumatoid factor in the blood helps distinguish psoriatic arthritis from rheumatoid arthritis.
Distinguishing features are not always present and the individual may have swelling of a few or many joints similar to other types of arthritis, making diagnosis difficult.
At what age and who does psoriatic arthritis affect?
- It may come on at any age.
- It is uncommon in children.
- Men and women are equally affected.
- 3 out of 5 (60%) men will develop arthritis of the spine as opposed to 2 out of 5 (40%) of women.
What is the outlook in psoriatic arthritis?
- Although psoriatic arthritis cannot be cured at present, many effective treatments exist.
- Treatments will depend on the severity of the disease, with some individuals having minimal arthritis while others are more severely affected.
- Psoriatic arthritis is a chronic condition, which can flare and go into remission (gets worse then better and then worse again and so on).
- Early diagnosis is essential in order to identify those who may develop more severe psoriatic arthritis and begin treatment that can prevent damage occurring to the joints. If you or a first-degree relative have psoriasis and you have the symptoms described in this leaflet (such as joint pain, stiffness, swelling or dactylitis), you should seek medical advice.
- If you are concerned you may have psoriatic arthritis something you could do for yourself is to complete the Psoriasis Epidemiology Screening Tool (PEST) questionnaire. To learn more about the PEST tool go to www.papaa.org/tools. A score of 3 or more out of 5 is positive and indicates a referral to rheumatology should be considered; your GP will be able to help with this.
- Only a small minority of individuals will go on to develop severe and widespread joint damage.
- Joints that are initially involved in psoriatic arthritis are usually the ones that continue to cause the problems at a later stage, though this is not always the case.
- Genetic markers to identify individuals with potentially more severe arthritis are now becoming practical and will help in identifying the most suitable type of treatment.
What is the treatment for psoriatic arthritis?
Although psoriatic arthritis is a chronic condition with no cure, there are many effective treatments to manage and control it. Some treatments for psoriatic arthritis may also help psoriasis of the skin. See What is Psoriasis? for further information.
Your psoriatic arthritis is likely to be managed by a number of healthcare professionals, which may include:
- your general practitioner (GP)
- a rheumatologist (joint specialist)
- a dermatologist (skin specialist)
- a specialist nurse
- a physiotherapist
- an occupational therapist
- a podiatrist (foot care)
- an ophthalmologist (eye specialist)
- a surgeon (joint replacement).
You may also be referred for specialist tests and imagery. These may include, when appropriate, x-rays, magnetic resonance imaging (MRI), ultrasound etc. Depending o n your individual circumstances you may be offered some of the following different types of treatments.
- Topical analgesic creams for the treatment of mild to moderate pain caused by arthritis.
- Topical medications for skin psoriasis such as vitamin D derivatives, although they may help the skin, have not been shown to benefit joints.
- NSAIDs (non-steroidal anti-inflammatory drugs) work by blocking the production of some of the body’s chemicals that cause inflammation and pain.
- csDMARDs (conventional synthetic disease-modifying anti-rheumatic drugs) are often prescribed in addition to NSAIDs to help slow down the biological processes that cause the persistent inflammation.
- Corticosteroids as joint injections can be very effective, although these do not work equally well in all individuals. They are safe when used in moderation and with precision.
- Targeted synthetic drugs (such as the PDE4 inhibitors), biologics or bDMARDs (such as anti-TNF, interleukin inhibitors (IL 12/23, IL17) and small molecules (such as the janus kinase- or JAK inhibitors) have been developed in recent years and may be offered if you do not respond effectively to other DMARDs. They act by mimicking the effects of substances made naturally in the human immune system.
- Seeking medical advice is vital about medications that can control inflammation and joint damage.
A severely inflamed joint should be treated with a period of rest followed by exercise (under medical supervision). Physiotherapy of joints and muscles which have stiffened can help prevent loss of movement. See Physiotherapy and exercise: Psoriatic arthritis
Remember: all treatments may have unwanted side effects or require special precautions (e.g. during pregnancy). Always make sure you have all the information before embarking on any course of therapy; this includes reading the patient information leaflets (PIL) provided with your medicines.
Does diet make a difference?
- No particular diet is uniformly effective; some people with psoriatic arthritis have found cutting down on saturated fats helps and may reduce the doses needed of other treatments, though research has not confirmed this.
- Dietary supplements such as evening primrose oil and certain fish oils may have a variable effect. They are safe and have other health benefits, but effects specifically beneficial to psoriatic arthritis have not been proven in research.
- Following guidelines about healthy lifestyle, keeping weight down and moderating alcohol intake are all generally accepted as beneficial regardless of having psoriasis or psoriatic arthritis. Reducing your weight to the healthy range (not being overweight or obese) has now been shown to improve arthritis, tendonitis and psoriasis. Furthermore, being a healthy weight also increases the likelihood of responding to medication. For more information see Psoriatic Lifestyle
Remember: many so-called cures for arthritis are not proven by clinical trials to be of use and may be driven by profit to those advocating them.
Does climate make a difference?
- Ultraviolet light helps psoriasis in some cases, otherwise climatic conditions such as the weather have a minor role to play; those whose skin and joints wax and wane together are usually better in summer than winter.
Does the severity of skin psoriasis matter?
- There is no correlation between the severity of the skin psoriasis and psoriatic arthritis.
What part do nails play in psoriatic arthritis?
- Nail changes are found in around 4 out of 5 individuals with psoriatic arthritis, compared with only about 2 out of 5 in those with psoriasis alone.
- Nail changes can be seen in both fingers and toes which can cause pain and makes using the hands difficult and walking can be affected sometimes.
- Nail changes include pitting and discolouration of the nail due to abnormalities in the growth of tissue in the nailbed.
- The risk of developing psoriatic arthritis is greater in individuals with severe psoriasis, yet severe psoriatic arthritis may occur with minimal skin disease.
Do we know what causes psoriatic arthritis?
- The cause of psoriatic arthritis is the subject of much research.
- You cannot catch psoriatic arthritis or psoriasis from someone else. Therefore, they are not contagious.
- The cause of psoriatic arthritis is not proven but experts believe it to be a combination of genetic, immunological and environmental factors. 2 out of 5 (40%) of people with psoriasis or psoriatic arthritis have a first-degree relative with the condition. This means you have a higher chance of developing psoriasis or psoriatic arthritis if you have a relative who has the condition. Some experts believe infections such as streptococcal infections may provoke psoriatic arthritis, though this is not proven.
- The role of bacteria in the gut (the microbiome) and developing psoriatic arthritis is the subject of current research.
- Trauma and stress may be contributing factors, although this is not proven.
- The genetic make-up of an individual is likely to determine the risk of developing psoriasis and psoriatic arthritis and probably influences the severity.
- Being overweight (obesity) is now understood to be linked to developing psoriatic arthritis and is the subject of ongoing research.
- There are certain genetic markers linked to the immune system which are now being used to predict the severity of psoriatic arthritis. Much more is known about the mechanisms that lead to inflammation in other conditions and it is likely advances in science will lead to much more effective treatments with fewer side effects.
Where can I get more information?
Around 9 out of 10 (91% as reported by the Office of National Statistics for 2019) UK adults have access to the internet – which is the easiest place to find more information. For those without internet access or who cannot get online, the options are becoming limited. A good place to start is the local public library, which often holds useful information. It may not be on immediate display, however, so try asking at the main desk. It is also worth asking your local GP surgery or hospital, which should have information in an accessible format.
Can I get financial support?
Many people worry about what happens if they cannot work or need financial help because of the effects of psoriatic arthritis. Fortunately for many, with good therapy and management the condition can be controlled and allow for a full and active working life.