Be part of the solution and make a difference
Getting a diagnosis

Be proactive!
When you develop skin or joint symptoms, it is easy to jump to the conclusion that you have a particular condition; this may be because you have read something in the media, on the internet, seen an advertisement, or a relative or a friend has a similar problem. Just because your symptoms are similar, do not assume that you have the same condition and therefore should be treated in the same way.
We all want to know what is causing a rash or pain, but it is not always as obvious as it might appear. Getting the correct diagnosis and then treating appropriately is very important.
Skin
If you have noticed a change in the appearance of your skin it can be worrying, but often there can be a simple explanation. The earlier you seek advice the easier it is to assess what may have caused the change, it could be an injury, allergic reaction or just a local irritation to clothing or activity.
Assuming the worst may cause unnecessary worry, and likewise, dismissing it as nothing may be inappropriate too. Sometimes seeking advice from a pharmacist may help or booking an appointment with your GP might explain the cause and provide a simple solution, either way there is help available to support your needs.
Problems with you skin can be embarrassing, but remember your doctor would have seen many cases before and early diagnosis can help to alleviate the anxiety and worry, not only for you, but also your family and those who care for you. Most skin problems can be treated effectively, but if you do not seek help, no one will know your skin is troubling you.
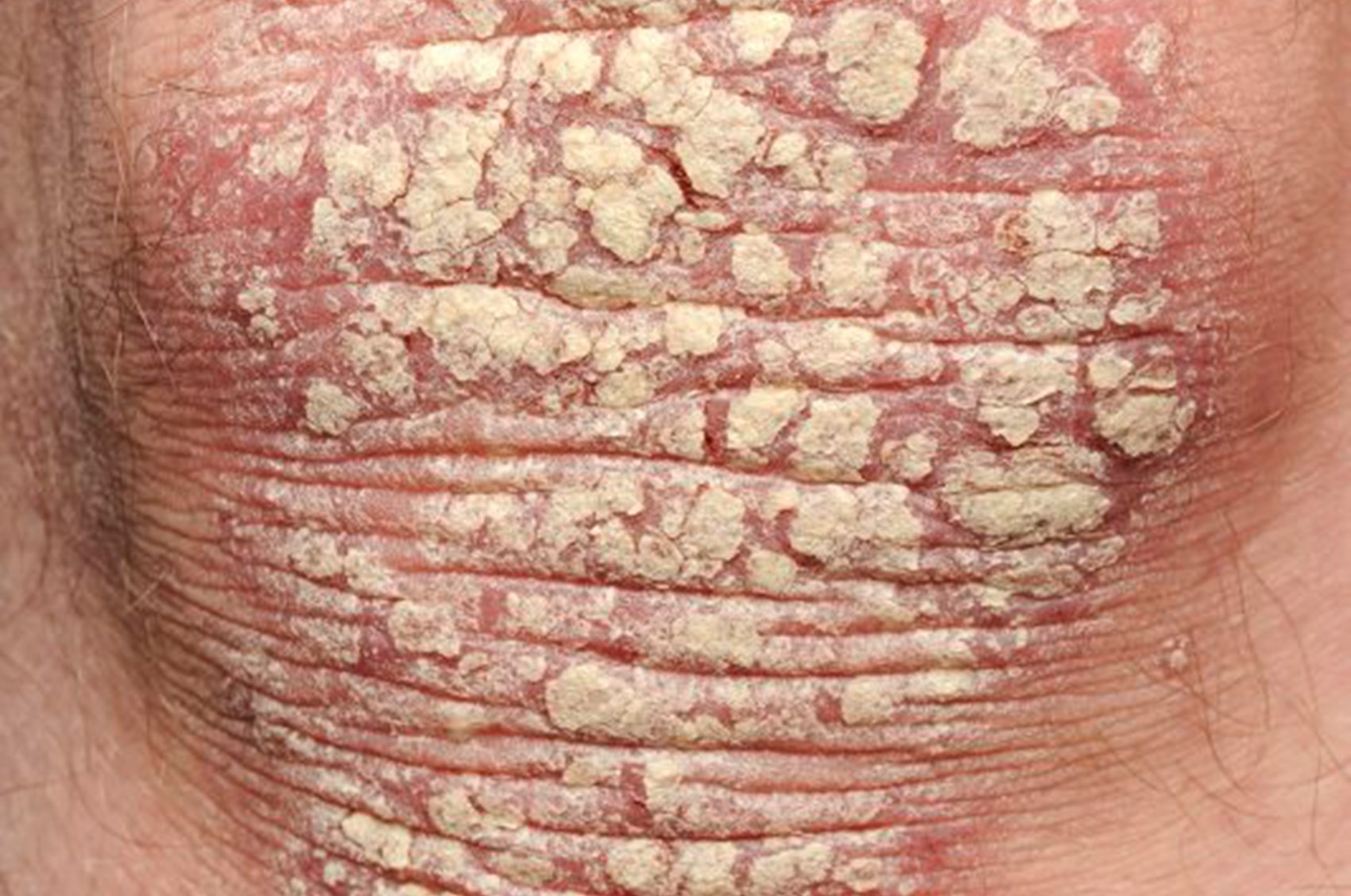
Diagnosing psoriasis
Diagnosis of psoriasis should be easy, and most cases are diagnosed upon visual examination by a GP, but not all psoriasis will be visible, so make sure your GP looks thoroughly, this will also help with determining severity and the appropriate course of treatment. You should try to remember when the symptoms started, if they appeared spontaneously or have developed over time. Try to recall if you had any other symptoms other than the rash, such as a cold, virus or sore throat, whether you experienced any trauma or stress. The more information you can provide will help to determine what the rash is or what might have caused it.
Psoriasis can sometimes look similar to other skin conditions, such as seborrheic dermatitis (seborrhea), dandruff, eczema, mycosis fungoides or pityriasis rubra pilaris, so in rare instances a small sample of skin (biopsy) might be sent for examination to rule out other conditions or to determine the exact type of psoriasis. It is important to get a correct diagnosis, so sometimes these further test may appear unnecessary, but can provide valuable data and to help reassure you.
Assessing severity
Once a diagnosis is established assessing the impact and severity can be more challenging. The use of various diagnostic tools (usually validated questionnaires) will aid in the process. One such tool is PASI (Psoriasis Area and Severity Index), although this is unlikely to be used at primary care level. More likely, the BSA (Body Surface Area) will be used, as it is easier to estimate. The area of the hand including fingers is equivalent to 1% of the total body area, so do not be surprised if the percentage that your GP calculates, appears to be lower than your own perception.
The use of quality of life surveys can provide useful guides to the impact and effect psoriasis has on daily life and mental well-being. Most commonly used are The DLQI (Dermatology Life Quality Index) and the HAQ (Disability Index of Health Assessment). If used correctly, these tools can provide an ongoing evaluation of disease influence beyond the visual symptoms. A list of diagnostic tools.
It is expected that once a diagnosis has been made that the process of assessment should follow those published by the National Institute For Health and Care Excellence (NICE) in guideline CG153 the Psoriasis: assessment and management, with the following recommendations being identified as priorities for implementation.
"Assessment tools for disease severity and impact and when to refer for specialist care
For people with any type of psoriasis assess:
- disease severity
- the impact of disease on physical, psychological and social wellbeing
- whether they have psoriatic arthritis
- the presence of co morbidities (other conditions).
Following assessment in a non-specialist setting (GP/primary care), refer people for dermatology specialist advice if:
- there is diagnostic uncertainty or
- any type of psoriasis is severe or extensive, for example more than 10% of the body surface area is affected or
- any type of psoriasis cannot be controlled with topical therapy or
- acute guttate psoriasis requires phototherapy or
- nail disease has a major functional or cosmetic impact or
- any type of psoriasis is having a major impact on a person's physical, psychological or social wellbeing."
If you are diagnosed with psoriasis, and not getting appropriate treatment, you may wish to remind your GP about what is recommended as best practice, as these guidelines are based on the best evidence available and designed to provide the best way of managing psoriasis for you and your GP.
Joint and muscle pain
Everybody at some stage in his or her life will have a pain in a joint or muscle. Deciding whether these pains are serious or just part of the rigours our body goes through can be difficult. Developing a pain or restricted movement can have a profound effect at any age, with fear and worries leading people to leap to conclusion that it is a serious problem or the reverse and dismiss as trivial.
If you develop any type of pain that persists for more than a few days it is worth seeking further assessment and advice. An appointment with a GP may allay any worries or fears, and you should not feel that it is a waste of time to report your symptoms, as doctors are there to help you.
Diagnosing psoriatic arthritis
Making a diagnosis of psoriatic arthritis, on the face of it should be easy. Many people when they do get a diagnosis will wonder why it was not obvious at the first appointment. However, there could be a number of reasons:
- lack of awareness of the condition
- variable non-specific symptoms
- no visible or psoriasis present
- lack of positive diagnostic test results (blood tests)
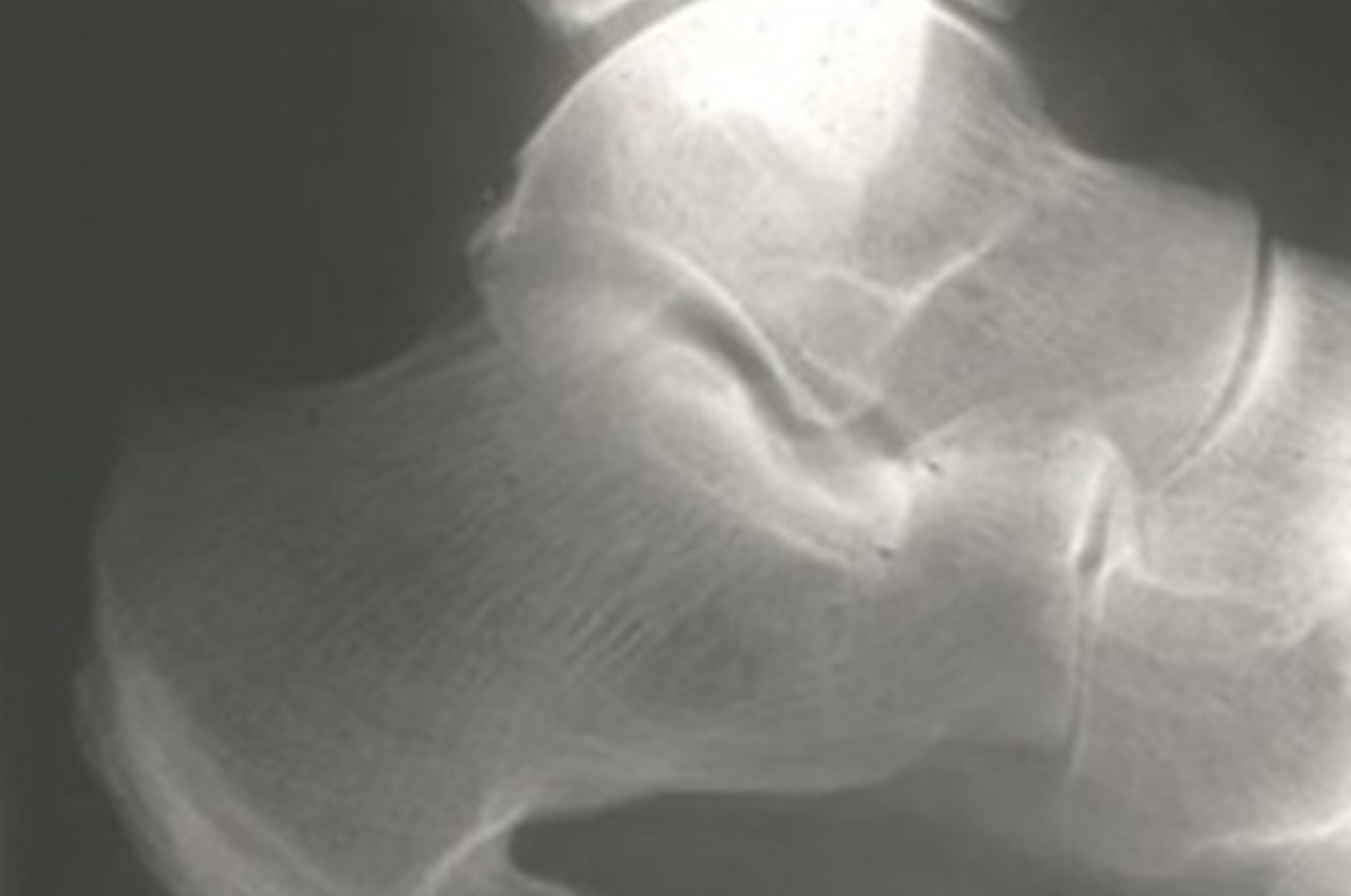
- no changes to basic x-rays and imagery
Although, there are symptoms that can point towards psoriatic arthritis, for many people the condition tends to develop slowly with aches and pains often in the hands or feet with stiffness in the joints, particularly in the morning, that then improves on movement. A family history of psoriasis could also provide a clue.
Age can provide another clue, as often the symptoms start between 20-30 years of age, which is not always the case for some other types of inflammatory arthritis.
Psoriatic arthritis can affect any joint; in some instances it can be just a single joint, which is swollen and painful for no obvious reason, changes to the nails are also potentially a sign that might suggest psoriatic arthritis.
Clinical examination and the elimination of other conditions is often how many people end up with a diagnosis of psoriatic arthritis. This can be a frustrating process, with numerous tests and visits, along with medication that may not provide symptom relief.
If you think that you may have psoriatic arthritis it is important to try to provide as much information as you can to your doctor, particularly the possibility of a link to psoriasis, as this could be the clue to unraveling the symptoms you are experiencing.