
A simple explanation
You have no items in your basket
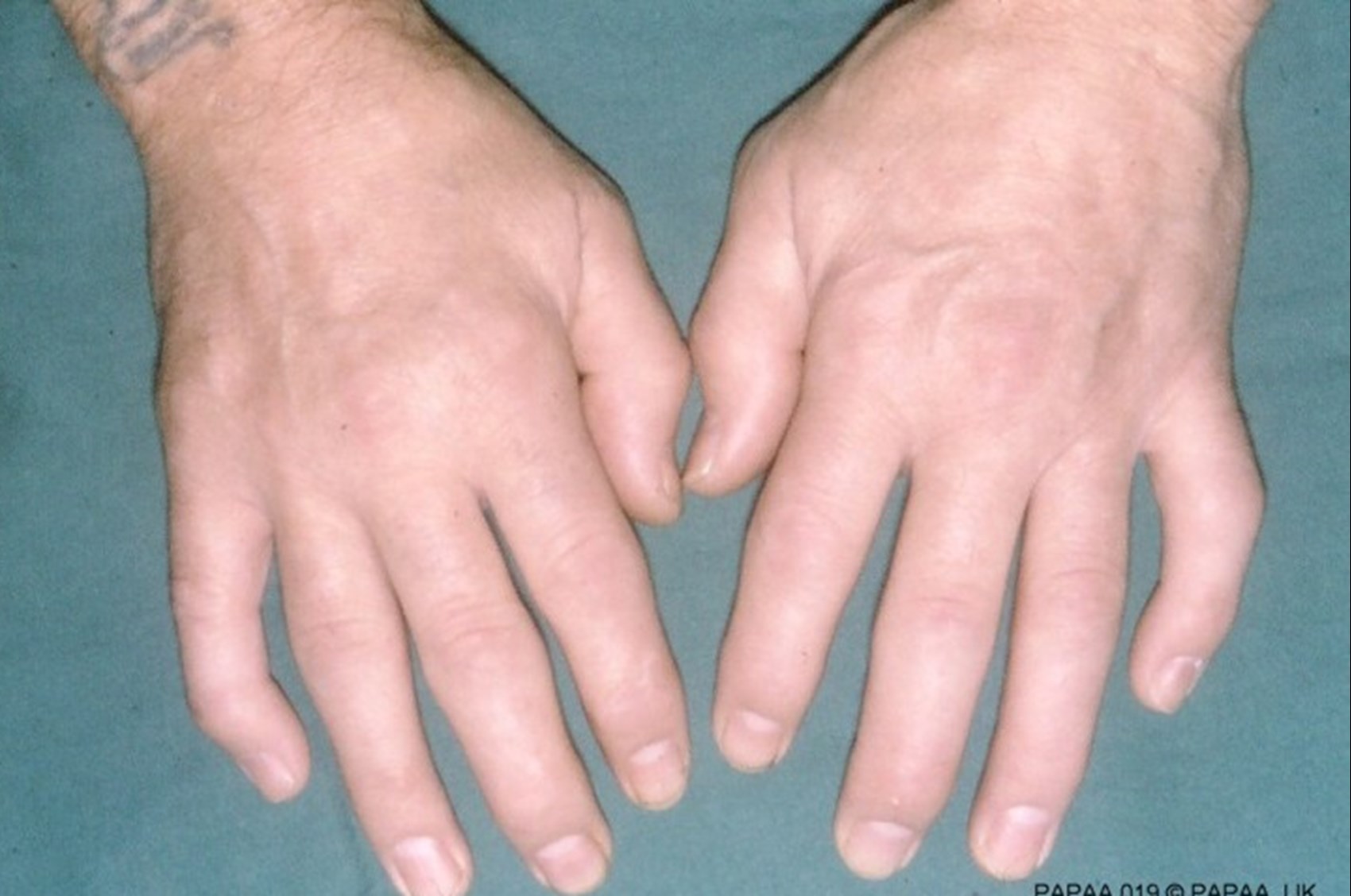
Pronounced sorry-attic arthritis also known as psoriatic arthropathy – sorry-attic arth-rop-athy.
Psoriatic arthritis (PsA) is a form of joint inflammation affecting individuals with the skin disorder, psoriasis. Affected inflamed joints can become tender, swollen and painful with movement. Sometimes the back becomes painful and stiff.
Skin psoriasis affects 1 in 50 people, which is about 1.3 million, or around 2% of the UK population. Out of this figure, around 30% of people with psoriasis may develop this form of arthritis.
In approximately 4 out of 5 (80%) of cases, the arthritis will develop after the appearance of psoriasis. However, in about 20% of cases, the joint inflammation will come first.
Psoriatic arthritis can be elusive and difficult to pin down to some of the medical profession, and indeed, you may feel sometimes that you have become a hypochondriac, experiencing the odd pains in your finger, toe, back or wrist.
Psoriatic arthritis can very much wax and wane, so if you book an appointment with your GP for a nagging pain in your toe or elsewhere, by the time you see the doctor, the pain could have moved to another joint or body part. So don’t worry, try to keep a mental note of any symptoms, aches and pains for a short while, then go to your GP.
The important fact to remember is that you must stress to your doctor that if you have psoriasis, no matter how small a patch there is, do inform the doctor of this because, psoriasis and psoriatic arthritis go together. This can be an important clue medically to diagnosing your condition early. The earlier the diagnosis, the better to prevent any unnecessary joint damage occurring.
If you feel you may have psoriatic arthritis you should firstly talk to your GP and explain to him your concerns and why you feel you may have psoriatic arthritis.
You may be lucky in that your GP spots all the early warning clues to your aches and pains, and diagnoses you correctly for prompt treatment options. However, there are still many people who are diagnosed much later due to lack of knowledge. This is not a criticism, but merely that GP’s have to have such a wide knowledge of many conditions and with psoriatic arthritis, it is not always as simple or obvious to diagnose.
A review of your medical history by your GP, symptoms, and blood tests to rule out certain other conditions are needed. Absence of rheumatoid factor in the blood often helps to distinguish psoriatic arthritis from rheumatoid arthritis.
Pitting of the finger nails, discolouration of the nail due to abnormalities in the growth of the tissue in the nail bed are always a certain clue of psoriatic arthritis presence. People with psoriatic arthritis almost always have nail involvement.
Your GP having taking into account your history and his own findings may then refer you on to a rheumatologist for confirmation. Indeed if you are under a dermatologist, they should be told of your various aches and pains immediately on a first visit or routine follow-up, as they will be able to diagnose psoriatic arthritis. So if you have any aches and pains, don’t forget to mention these, they may then cross refer you to a rheumatologist for treatments to be prescribed.
Psoriatic arthritis can affect your fingers, wrists, spine, feet, eyes (uveitis) and or neck. You may at some time experience tender, inflamed muscles and tendons, especially around these areas.
As many as 12,000 children in the UK are affected by arthritis. It is known as juvenile chronic arthritis (JCA), of which there are three main types, still’s disease, polyarticular juvenile chronic arthritis and polyarticular onset juvenile chronic arthritis. Psoriatic arthritis is a minor subset of JCA and is uncommon.
There are 78 major joints in the body and psoriatic arthritis can affect any one of these. Usually, however, certain joints are more likely to be affected (such as fingers and toes). Different patterns are found. Sometimes just one or two joints (such as a knee or ankle) are a problem but often several joints, both large and small and on both sides of the body, are involved. About a third of people with psoriatic arthritis also have spondylitis which can result in a painful, stiff back or neck. Psoriasis can affect the nails with pitting, discolouration and thickening and this may be associated with inflammation in the joints at the end of the finger or toe. Another way in which psoriatic arthritis can be recognized is the finding of a sausage-like swelling of a finger or toe, called dactylitis. This is caused by inflammation occurring simultaneously in joints and tendons, painful heels and other bony prominence can also occur and this is caused by inflammation where gristle attaches to bone.
Apart from the skin, nails and joints, increased cardiovascular morbidity is considered part of psoriatic disease, as is the association with inflammatory bowel disease. An itchy, red eye due to conjunctivitis is more common in people with psoriatic arthritis and some people occasionally develop a painful, red eye caused by inflammation around the pupil of the eye, which is called iritis or uveitis. Anaemia (not enough red blood cells) may also be found but this is the result of long-term inflammation and is not a specific feature of psoriatic arthritis.
To make a diagnosis of psoriatic arthritis most doctors would require you to have psoriasis, or a history of psoriasis in a close relative, together with arthritis and inflammation in at least one joint. If several joints are affected the doctor would expect to find a pattern of joints involved which matches one of the patterns usually seen in psoriatic arthritis. Blood tests for rheumatoid arthritis are usually negative but often blood tests of general inflammation in the blood are positive. These latter bloods are called the erythrocyte sedimentation rate (ESR) C-Reactive protein (CRP) or plasma viscosity (PV) all are measures of inflammation and abnormal, if the value exceeds a certain level.
You can expect to have regular blood tests to monitor the amount of inflammation in your blood and to monitor the effect of any treatment you will be given. X rays will be taken from time to time and you may also have ultrasound scans and MRI scans.
If you have psoriasis and or psoriatic arthritis it means that it is highly likely you will have a genetic predisposition. It is possible that other close family members will have it too such as sibling, parent, grandparent etc. but this doesn’t always follow. Developing the condition has nothing to do with your lifestyle, not looking after yourself, physical job etc.
Research suggests that something (perhaps an infection) acts as a trigger in people who are susceptible because of their genetic make-up. Psoriasis often runs in families, as does arthritis. A particular combination of genes makes some people more likely to get psoriasis and psoriatic arthritis. It is likely that a variety of infections (including bacteria that live in patches of psoriasis) can trigger the disease.
Let’s face it too much stress does not do anyone any favours. So the less stressed you are the better you will be. There is much research being done with psoriasis patients to see what effects stress actually has, there are always conflicting views on the subject.
Unlike rheumatoid arthritis where you do get set patterns of the disease, psoriatic arthritis can be more elusive in its patterns of progression. It can wax and wane, disappear or flare-up for long or short periods of time.
The long-term prognosis for the management of psoriatic arthritis is good, especially if it is diagnosed early and correctly, with a treatment regime provided by your rheumatologist. However, if it has been a few years before you have been diagnosed, don’t worry, there are still good treatment outcomes. With good treatment compliance management, lifestyle changes if necessary, positive outlook and plenty of future research and developments coming through, the future is not as bleak as you think.
Yes, this can be perfectly normal, everyone is different and our bodies cope in different ways, don’t worry. You may have short/long bouts where you feel incredibly tired, then perk up again. Be kind to yourself and go with these periods of tiredness, resting where your can.
Yes, this is a very normal process, a form of mourning and coming to terms with the fact that you have arthritis, and some things may have to change in your lifestyle to compensate, making things easier for you. Don’t panic, try to work through your feelings, talking with a partner or someone close to you, If the feelings don't pass, see your doctor who may be able to refer you to some form of short-term counselling.
Psoriatic arthritis is not strictly hereditary, but there is a genetic contribution, that is to say, you have to have a predisposition towards it. The genetic make-up of an individual is likely to determine the risk of developing psoriasis and arthritis and probably influence the severity. There are certain genetic markers linked to the immune system which are now being used to predict severity of psoriatic arthritis.
Don’t be too hard on yourself – that means don't feel guilty because on some days you can’t be as active as others. Psoriatic arthritis can affect any age group, not just those in later life! Just because you may look fit and well to others, is not a reason for you to justify yourself to them when you are feeling unwell.
Good compliance with your medications is key, as is keeping up with regular hospital visits with your rheumatologist and dermatologist.
Make sure you get the best out of your hospital visits in the time allocated to you. Go over in your head the things you need to get covered in the consultation. Make sure you know of all the side effects on treatment options offered to you – talk these over with your consultants and specialist nurses at the hospital clinics.
Try to keep a positive approach to your illness, learn to live alongside it.
If you need to talk about your feelings, make sure you do, choose a caring person you can relate to. Sometimes a problem shared is indeed a problem halved.
If you feel you need some support, ask a family member or a friend to come with you to the hospital appointment. This can sometimes be very helpful, if the doctor is firing questions at you, there may be some things you forget, that a partner can help with too. Make it a team effort, feel supported. Remember you are always entitled to get a second opinion if you are unsure about previous medical advice given.
You can get help and advice with the management of pain. Your hospital may run pain management clinics or have specialist nurses that can give effective advice on how to relieve bad bouts of pain.
There are various books you can read on the subject, as indeed there are various gadgets that can also help with temporary relief – i.e. TENS machines. Have a chat when you next visit the hospital, or indeed ask your practice nurse at the GP surgery.
There are now many treatment options available to people with psoriatic arthritis, some options will have to meet certain criteria before being offered, but there are many to be tried and tailor-made to the patient’s needs.
The treatments range from:
There are always side-effects with any drugs either topical, oral or intravenously for any illness. Drugs used for both the treatment of psoriasis and psoriatic arthritis are no exception. So make sure you discuss fully any medications with your doctor or specialist nurses. You can then make informed choices about your condition and how they will affect you and your lifestyle.
Some drug treatments may make psoriasis worse, but then again, some can also make it better too. Before you start any treatments offered, discuss this both with your dermatologist and rheumatologist. DON’T FORGET to politely request that both consultants let each other know of your treatment regimes, this helps both of them evaluate your treatment and any side effects that you may be likely to experience. Some people find that when their psoriasis is bad their arthritis is also bad and as one improves, so does the other. This most often occurs when the skin and joint disease start simultaneously. Some of the arthritis treatments also help the skin (methotrexate is an example) and this is can help the doctors decide which is the best drug to use.
Treatments may take a certain amount of time before you see and feel benefits. Ask your doctor when you should expect to feel better.
There are many consultants and specialist GPs that have an interest in psoriasis/psoriatic arthritis, and some may even have special clinics running within hospitals for psoriatic arthritis so it is worth doing some research locally to see if this is the case, or ask your GP.
Initially your GP is the first point of contact, who then should refer you on to a dermatologist/rheumatologist, if this is not already the case. If you are not happy with the advice you receive, remember you are always entitled to seek a second opinion. Remember, If you are seeing a dermatologists for your psoriasis and a rheumatologists for your arthritis make sure each is aware of this, so they can liaise and provide you with appropriate care for both conditons.
A full case history will be taken, urine and blood tests requested, x-rays, sometimes specialist x-rays, images and scans may also be requested, plus a full examination of your affected parts i.e. back, hands, feet etc.
Ask about your medicines:
Be wary about following fad diets especially if the diet recommends stopping your tablets in order to try the diet. Don't do this without telling your doctor. Sometimes the diet can help reduce the need to take some of your tablets but unfortunately this is rare. Cod liver oil and other marine (sea water) fish oils may reduce the amount of anti-inflammatory drugs needed to control joint inflammation and therefore may be worth a try. There is no evidence that glucosamine or chondroitin help with this condition. See our lifestyle and nutrition information.
If you are overweight, you need to follow a weight-reducing diet because of the extra strain this puts on your leg joints and back.
Check with your GP or consultant as some drugs may be affected by alcohol consumption. Following alcohol guidelines is always a wise choice.
Many complementary therapies, such as reflexology, reiki, indian head massage, aromatherapy and pilates are unproven in the treatment of psoriatic arthritis. However, they are unlikely to do any harm and may improve your general well being and how you feel about yourself. If you are going to try complementary and alternative medicine (CAM) then consult your healthcare provider.
Psoriatic arthritis will not in itself affect your chances of having children or carrying a successful pregnancy. For a woman who becomes pregnant, the arthritis often improves during the pregnancy. However, the arthritis may worsen after the child has been born. It is also worth remembering that looking after small babies is hard work and even harder if you have painful joints. Would-be mothers with psoriatic arthritis should therefore try to get plenty of help with childcare. Sexual intercourse may be painful, particularly for a woman whose hips are affected. Using different positions can help. It may help to discuss this with a member of the rheumatology team.
Some of the drug treatment given for psoriatic arthritis should be avoided when starting a family. For instance, sulphasalasine can cause a low sperm count (this is not permanent) and methotrexate should not be taken by couples trying to conceive. If you are considering starting a family you should discuss your drug treatment with your doctor.
If you are of childbearing age, either male of female and have not considered starting a family, but would like to in the future, you should always make this clear to your doctor. This may have a significant bearing on the treatment options made available to you. There are risks and side-effects with certain medications that may interfere with conception or pregnancy – discuss this fully with your doctor, it is important that both parties know the correct facts about your intentions for the future so as to avoid delays in conception or other facts that could influence your future decisions.
Since 2010, talking therapies which include counselling, cognitive behavioural therapy (CBT) and psychotherapy have been made more widely available within the NHS for a variety of conditions. If your GP or another healthcare professional thinks that you will benefit, and refers you to a qualified counsellor, it may be free of charge.
It is hard to generalise on how much exercise is best - no two people are the same. However, inflammation can cause generalised tiredness and you may find you need to take more rests than usual. On the other hand, inflammation also causes muscle weakness and stiff joints and it is very important to keep exercising the joints to stop them becoming weaker and losing function. It is a question of finding the right balance for yourself but remember not to neglect either rest or exercise when you are trying to help your disease.
There is no reason why you should avoid any activity that you previously enjoyed, but remember that there may be times when you do feel unable to complete a task, or your arthritis is in a ‘flare’.
Sometimes it can be hard for those close to you to understand how psoriatic arthritis affects you. They may get angry with you or feel frustrated, but in any relationship there is a need for ‘give and take’ and discussing your feelings might help.
There shouldn’t be any reason why you cannot continue to work, employers cannot legally discriminate against you because you have psoriatic arthritis, and may need to adapt your work to suit your condition
Having psoriasis and/or psoriatic arthritis can cost you a small fortune each month, having regular prescriptions. You can reduce your outgoings on prescriptions by having a pre-paid prescription card.
The best place to find out all the latest information is by visiting the Direct Gov website, where you will find out what you have to do to make a claim.
Can surgery help improve my mobility in my wrists, finger joints, back etc?
Surgery is not often needed in psoriatic arthritis, although sometimes operations are necessary to repair damaged tendons and in more severe cases joints may need to be replaced. However, if psoriasis is present in the skin around the affected joint some surgeons are wary about performing a surgical procedure.
No, there is no cure for either psoriasis or psoriatic arthritis. Although, there are many who proclaim to have a cure, you should treat these claims with firm scepticism.
Today there is much more known about the mechanisms that lead to inflammation in other conditions and it is likely advances in science will lead to much more effective treatments with fewer side-effects.
There is a great deal of research looking at the causes and treatments of both psoriasis and psoriatic arthritis.