
A simple explanation
You have no items in your basket
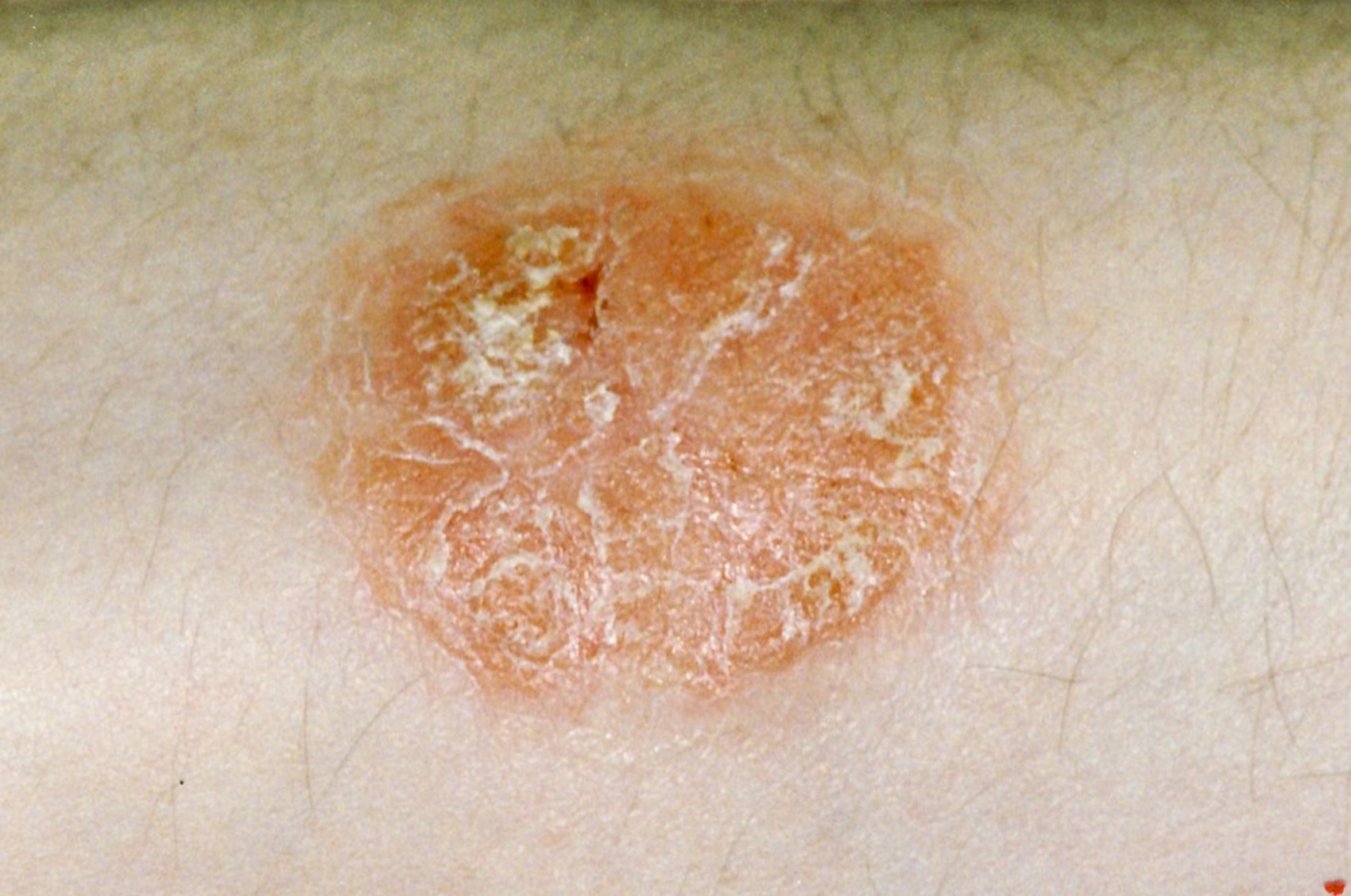
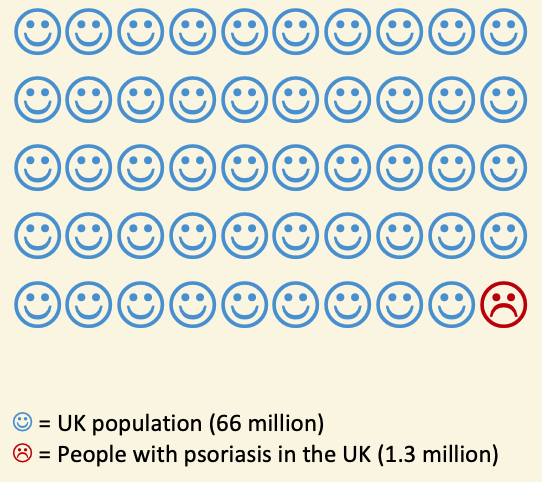
Psoriasis (sor-i’ah-sis) is a long-term (chronic) scaling disease of the skin which affects around 1 in 50 people, which is about 1.3 million, or around 2% of the UK population. IT IS NOT CONTAGIOUS and you cannot catch psoriasis from someone else.
It usually appears as red raised, scaly patches, known as plaques. In people with skin of colour, the redness is less pronounced, and psoriasis may appear as violet or darkened areas of skin. The plaques therefore may appear darker, brown or as purple patches with grey scales.
Any part of the skin surface may be involved but the plaques most commonly appear on the elbows, knees and scalp. It can be itchy but is not usually painful. Nail changes, including pitting and ridging, are present in nearly half (40%-50%) of all those who have psoriasis.
There are many different types of psoriasis, including chronic plaque psoriasis, types of pustular psoriasis (all of which are described in this leaflet), guttate psoriasis, scalp psoriasis, flexural psoriasis, napkin psoriasis, nail psoriasis and erythrodermic psoriasis (a rare, serious condition which can affect the whole body).
For those that have psoriasis around 1 in 4 may develop an associated psoriatic arthritis (PsA), which is about 325,000 people, or around 0.5% of the UK population. PsA causes pain and swelling in the joints and tendons, accompanied by stiffness particularly in the mornings. The most commonly affected sites are the hands, feet, lower back, neck and knees, with movement in these areas becoming severely limited.
Not all people will be affected in the same way and doctors will class the condition as mild, moderate or severe.
Remember, although psoriasis is a chronic condition, it can be controlled and go into remission (go away, often temporarily and sometimes permanently).
Mild psoriasis which is the most common presentation, accounts for around 1 million people in the UK or 4 out of 5 of those affected (80%). With mild psoriasis, people will have a few patches. Typically may not be visually obvious or noticeable but may still need to be treated and generally is not likely to cause problems and can be easily controlled.
Moderate psoriasis is when more skin is affected and visually it becomes more obvious. Around 200,000 people in the UK have moderate psoriasis which is about 3 out of 20 of those affected (15%). Moderate psoriasis is more widespread but, again, can usually be controlled with self-management under the supervision of a GP or nurse.
Severe psoriasis begins to become more of a problem for those affected which is about 65,000 people in the UK or 1 out of 20 (5%). When psoriasis becomes severe, large areas become covered with psoriasis; the condition becomes difficult to self-manage or no longer responds to treatment. At this stage referral to secondary care at a local hospital outpatient department, or in extreme cases, an inpatient stay may be felt necessary in order to provide the most suitable (optimum) care and monitoring.
Normally a skin cell matures in 21 to 28 days. During this time it travels to the surface of the skin, where it is lost in a constant, invisible shedding of dead cells. In patches of psoriasis the turnover of skin cells is much faster, around four to seven days, and this means that even live cells can reach the surface and accumulate with dead cells. It is thought that cells in the immune system (T cells) become overactive, leading to rapid growth of skin cells and the formation of psoriatic plaques. The extent of psoriasis and how it affects an individual varies from person to person. Some may only be mildly affected with a tiny patch hidden away which does not bother them, while others may have large, visible areas of skin involved that significantly affect daily life and relationships. The process is the same wherever it occurs on the body. There are some factors that trigger flares of psoriasis including infection, stress, alcohol and smoking. Obesity is also linked to psoriasis and maintaining a healthy weight can reduce the severity of the disease.
It affects men, women and children alike. It can appear at any age in varying degrees but usually between the ages of 10 and 30. The severity of the disease varies enormously, from a minute patch to large patches covering most body areas. Psoriasis can also run in families and it is known that the disease is multi-genetic (a condition where several genes may each have different roles, contributing to specific characteristics of disease) and therefore children may not necessarily inherit psoriasis. It is estimated that if one parent has psoriasis then there is a 3 out of 20 (15%) chance that a child will develop the condition. If both parents have psoriasis this increases to about 15 out of 20 (75%). Interestingly, if a child develops psoriasis and neither parent is affected there is a 1 out of 5 (20%) chance that a brother or sister will also get psoriasis. This is because the condition is known to skip generations, so somewhere there will be a familial link to a relative via one or both parents.
There is no cure at the moment. However, as a consequence of current research, our understanding about what happens in psoriasis is growing and new drugs are being developed. In the meantime, there are a number of treatments that are effective in keeping psoriasis under control.
The art of treating psoriasis is finding the best form of treatment for each individual. There is no single solution that is right for everyone.
In the absence of a cure you will always have psoriasis, but this does not mean that the signs will always be visible. Normally, the rash tends to wax and wane (increase and decrease). There will be periods when your skin is good, with little or no sign of psoriasis. Equally, there will be times when it flares up. The length of time between clear skin and flare-ups differs for each individual and is unpredictable. It may be weeks, months or even years.
Chronic plaque psoriasis: Raised, red, scaly patches mainly occurring on the limbs and the trunk, especially on the elbows, knees, hands, around the navel, over the lower back (sacrum) and on the scalp. The nails may be affected so that they become thickened and raised from their nail beds, and the surface of the nail may be marked with small indentations (pits). This is the most common type of psoriasis, affecting approximately 9 out of 10 people with psoriasis.
Guttate psoriasis (raindrop psoriasis): So named because it manifests itself over the body in the form of scaly, droplet-like patches. Numerous small, red, scaly patches quickly develop over a wide area of skin, although the palms and the soles are usually not affected. It occurs most frequently in children and teenagers, often after a throat infection due to streptococcal bacteria. Some people who have had guttate psoriasis will go on in later life to develop chronic plaque psoriasis.
Scalp psoriasis: Raised, red, thick, scaly plaques on the scalp and around the hairline. It is common and approximately 1 out of 2 (50%) of all people with psoriasis have it on their scalp. The reason it deserves special mention is that it can be particularly difficult to treat and usually requires specifically formulated medicines. It is awkward to treat with creams and ointments because the hair gets in the way. See Scalp psoriasis for more information
Flexural psoriasis: Produces red, well-defined areas in skin folds (flexures) such as the armpits, between the buttocks and under the breasts .Scaling is minimal or absent. This type of psoriasis can be frequently irritated by rubbing and sweating due to its location in the skin folds and other tender areas. Such areas can also be prone to yeast or fungal infections, which might cause confusion in diagnosis. Go to sensitive areas article.
Napkin psoriasis: Develops in the nappy area of an infant to cause a bright red, weeping rash or more typical psoriasis plaques. A child who has napkin psoriasis as a baby does not seem to have a higher risk of developing other forms of psoriasis in later life.
Palmar plantar pustular psoriasis: Small, deep seated pustules form that usually only affect the palms and soles. Pustules are caused by the accumulation of white blood cells and are not infected. See Pustular psoriasis for more information
Generalised pustular psoriasis: In rarer cases, the pustules are more widespread and accompanied by a fever. The development of generalised pustular psoriasis requires urgent hospital treatment.
Erythrodermic psoriasis: A rare, serious condition where skin redness (erythema) can affect the whole body. Dilated blood vessels in the skin affect blood circulation to other parts of the body, with problems of fluid balance and rapid heat loss. In severe cases, this may be life-threatening. Erythrodermic psoriasis is very rare, with approximately 200 to 300 new cases in the UK each year. These patients need very intensive specialist care in hospital.
Nail psoriasis: About half of those with psoriasis (40% to 50%) will have involvement of the nails. In some individuals with psoriasis this may be mild and very minor involvement. The fingernails and toenails are affected equally. This may just be one nail, or all of them. Discolouration, pitting and separation from the nail bed (onycholysis) are the most common characteristics of activity. Nails can be a good indicator that psoriasis is present and can help the doctor to diagnose if an associated form of arthritis is present. See Nail psoriasis for more information
Psoriatic arthritis (psoriatic arthropathy): 1 in 4 (around 25%) of people with psoriasis may develop an associated arthritis called psoriatic arthropathy, which causes pain and swelling in the joints and connective tissue, accompanied by stiffness particularly in the mornings and when rising from a seat. Most commonly affected sites are the hands, feet, lower back, neck and knees, with movement in these areas becoming severely limited. Chronic fatigue is a common complaint linked with this condition. If you are experiencing mild aches and pains and have psoriasis, even very mildly, consult your dermatologist for further advice and if necessary a referral to a rheumatologist for further assessments. For more detailed information on psoriatic arthritis see What is Psoriatic Arthritis?
There may not be a cure yet but there is much you can do to help maintain and control your psoriasis. Psoriasis, regardless of location or type, is often irritated by contact, particularly tight clothing such as elasticated waistbands, socks, tights, and underwear. It may be useful to wear looser clothing where psoriasis is likely to be irritated either when flaring or during periods of treatment. Identifying factors (e.g. stress, alcohol) that may cause your psoriasis to flare, using a diary, can be helpful.
Yes, there are many forms of treatment for psoriasis, which range from those you apply to the skin (topical) to tablets, and more recently injectable therapies, See Treatments for Psoriasis.
Many people who have psoriasis find that the sun and artificial ultraviolet light (UV) helps to improve their skin’s appearance. For some the change is dramatic. Be aware that exposure to the sun and artificial UV therapy can cause damage to the skin. See Psoriasis and the sun and Psoriasis and phototherapy
For some people, talking therapies such as cognitive behaviour therapy (CBT) can also help them understand the psychological impact of psoriasis and provide a safe therapy which may help them cope with psoriasis. See our free online CBT programme
Your general practitioner or dermatologist will be best placed to advise you and keep you informed of all current and new treatments available and to recommend the best treatment programme for you personally.
Remember: Your treatment can only be as good as you allow it to be - that means if the treatment takes six weeks, you have to follow it as instructed for six weeks and no ducking out! Adherence to treatment instructions is an essential part of managing your psoriasis.
A healthy diet is important for wellbeing and can reduce your risk of many long-term illnesses. However, there is no clear link between what you eat and the severity of psoriasis symptoms.
See Psoriatic Lifestyle for more information
If you think you have psoriasis, go and see your GP. He or she may decide themselves to start treatment or refer you to a dermatologist for advice.
Don’t forget, if you are also experiencing aches and pains in any of your joints, have any other symptoms or if you have a family history of psoriasis, inform the doctor. This will assist with diagnosis and treatment.
Remember: All treatments may have unwanted side effects or require special precautions (for example, during pregnancy). Always make sure you have all the relevant information available before embarking on any course of therapy. This includes reading the patient information leaflets (PIL) provided with your medicines.
Lots of people worry about what happens if they cannot work or need financial help because of the effects of their condition. Fortunately for many, with good therapy and management their condition can be controlled and allow for a full and active working life. But if you do find that even for a short period of time you are likely to need help, visit the national government websites online.

If it is easier, contact your local government or council office, where you should be directed to the appropriate resource and information. If you require regular prescriptions, you may save money with a prescription prepayment certificate so it is worth speaking to your pharmacist about this.
Always consult your doctor or healthcare provider.
This article is adapted from the What is Psoriasis? leaflet.