
Search
You have no items in your basket

The feet are an important part of the human anatomy; each foot has 26 bones, 33 joints and is controlled by muscles, tendons, and ligaments. The skin on the sole of the foot is different to that on the rest of the body, with a particularly large number of sweat pores.
To cope with the weight that is continually placed on them, the soles of the feet have the thickest layers of skin on the human body. They are, however, very sensitive and act as sensors when walking or standing. Therefore, anything that interferes or affects the feet can have a profound impact on function and general wellbeing.
Most commonly, psoriasis on the foot looks similar to plaque psoriasis in other locations on the body and is called palmoplantar psoriasis. Often the plaques are thick and scaly, which can be painful and bleed if cracks appear. It is important to distinguish psoriasis from other conditions that affect the foot.
Apart from plaque, there are other types of psoriasis which affect the foot and have a different appearance.
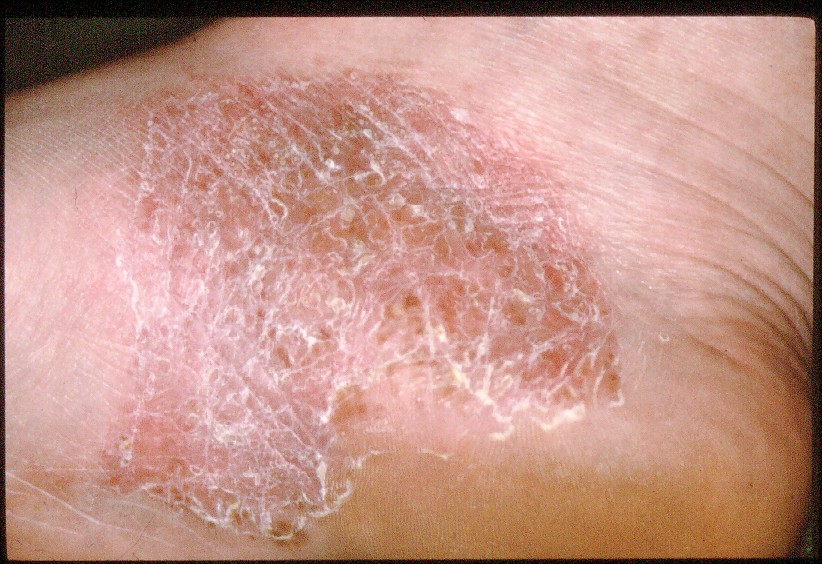
Localised pustular psoriasis – also known as palmoplantar pustular psoriasis (PPP) – affects about
Localised pustular psoriasis also known as palmoplantar pustular psoriasis (PPP) – affects about 5% of people with psoriasis. It occurs most commonly between the ages of 20 and 60. It can be painful and is more common in women than men. About 10-25% of people with PPP have a family history of psoriasis but the precise reason why some people develop it is not known.
PPP causes pustules on the palms and soles. As in all types of psoriasis, infection and stress are suspected trigger factors. PPP is normally recognisable by yellow/ white pustules approximately 2-3mm in diameter, appearing on fleshy areas of hands and feet, such as the base of the thumb and the sides of the heels.
These pustules are sterile, which means they are not the result of infection. Antibiotics do not affect them. After time, the pustules dry up and resolve, leaving brown stains on the skin surface. The natural history of the disease is usually cyclical (occurring often or repeatedly), with the appearance of new crops of pustules followed by periods of low activity in which the pustules resolve. See Pustular psoriasis.
Acrodermatitis continua of Hallopeau is a very rare form of localised pustular psoriasis. This looks similar to palmoplantar pustular psoriasis, but is localised to the ends of the fingers and, less commonly still, the toes (acropustulosis). It usually starts after some trauma to the skin. It tends to be painful and frequently affects the nails. It may lead to loss of the nails. Bone changes can be seen in severe cases. It is difficult to treat and many therapies have been tried. Topical treatments are usually not very successful but occasionally systemic medications may help to clear the lesions and restore the nails.
Given they are part of the skin, it is perhaps not surprising that nails can be affected by a skin disease such as psoriasis. Nail psoriasis is very common, yet no one knows why some people get nail involvement and others do not. Nails grow from the nail plate, which is just under the cuticle. In people who develop psoriasis of the nails, it is involvement of the nail plate that causes pitting, ridging, thickening, lifting and discolouration of the nail due to abnormalities in the growth of tissue in the nail bed.
The nail is made of modified skin and, once it has grown, it can only be altered by filing or clipping. Treatments are usually directed at the nail bed or the nail folds that tuck around the edges. Treated inflammation in these tissues can result in better nail growth with fewer features of psoriasis, but treatment of nail psoriasis can be difficult. See Nail psoriasis
It is not fully understood what causes psoriasis, but it is an inherited inflammatory disease. It can be triggered by events, illness or injury to the skin. A particular process known as Koebner’s phenomenonor Koebnerisation is named after the German dermatologist Heinrich Koebner. Koebner found that people with psoriasis whose skin became traumatised following an injury, often developed a psoriatic lesion in the area, but where psoriasis had not previously been seen; such sites include cuts, bruises, burns, bumps, vaccinations, tattoos and other skin conditions.
If you think you may have psoriasis on your foot or feet, it is best to get a diagnosis. Visiting your GP or asking your pharmacist is a good place to start. Alternatively, you may wish to see a local chiropodist (sometimes known as a podiatrist), particularly if your nails have become thickened and difficult to manage.
Psoriasis on a foot or both feet may be diagnosed by simple examination, but if there is any doubt then referral to a specialist (dermatologist) may be required. It is unlikely that any specific test will be performed unless there is a suspicion of a fungal infection, when some samples may be taken for laboratory analysis.
For plaque psoriasis on the foot, treatment will generally be similar to those recommended for other areas of the body, with the use of topical (applied to the skin) creams, ointment and gels. See Treatments for psoriasis.
The use of phototherapy (ultraviolet light) may be considered, but availability and access to appropriate centres can sometimes be limited. It may be possible to treat psoriasis affecting the hands and feet with localised phototherapy. See Psoriasis and phototherapy.
Palmoplantar pustular psoriasis is often difficult to treat, although some people do benefit from potent topical steroids combined with tar preparations. However, in most cases treatment with acitretin (a vitamin A derivative) tablets is the most effective.
Treating nails can be problematic, as once the nail changes appear the damage has already occurred. It is important to check that other conditions that affect the nail, such as fungal infection, are not present, as these can often look similar to nail psoriasis. It is advisable to keep nails short and clean. See our leaflet Nail Psoriasis. See Nail psoriasis.
The ankle is a hinge joint between the talus bone of the foot and the two bones of the lower leg, the tibia and fibula. The ankle joint lets you move your foot up and down. Other movements, such as tilting and rotation, occur at other joints in the foot itself. Each foot contains 26 bones which form joints where they meet. These joints are all lined with a synovial membrane that produces lubricating oil. Many tendons pass around the ankle to connect the bones with the muscles that move them. These are also covered in synovial membrane and oiled with synovial fluid. In psoriatic arthritis, any part of the foot can be affected and become inflamed and painful, which in turn may lead to permanent disability.
The synovial membranes that line joints, tendons and connective tissue become thickened and inflamed (tendonitis and enthesitis). This releases more fluid than normal so the joints and tendons become tender and swollen, which may result in:
The pattern of joints that may be involved can vary from person to person, and may just affect a small number of joints (oligoarthritis) or many joints (polyarthritis). Most commonly, psoriatic arthritis is asymmetric in pattern (not identical on both sides) unlike rheumatoid arthritis, which is symmetrical.
In terms of symptoms, psoriatic arthritis can cause stiffness in the joints, particularly after a period of inactivity such as after waking up in the morning. Psoriatic arthritis can also cause swelling of an individual toe so it looks like a sausage, called dactylitis. Some people also experience heel pain because the Achilles tendon, which connects the calf muscles to the heel bone, has become inflamed. Swelling around the ankle is common in psoriatic arthritis affecting the foot.
Psoriatic arthritis can lead to shortening or clawing of the toes, hyperextension of the big toe and some in-rolling of the ankle with flattening of the metatarsal arch. Stiffness of the joints, rather than instability, also happens quickly and can become irreversible within a few months. The occurrence of calluses and ulcers on the soles of the foot is less common than in rheumatoid arthritis (RA) but corns over the interphalangeal joints can be very painful.
Symptoms tend to flare up and then die down again. If the inflammation is persistent and left untreated, toe joints can fuse together, with the space between the individual joints being lost.
You should always seek medical advice if you experience stiffness in your joints especially after inactivity, severe pain, redness or swelling in one or both feet, whether this is mild or severe. It is essential to minimise the inflammation to avoid permanent joint deformity.
As with skin psoriasis, the cause of psoriatic arthritis is unknown, with an event or illness often considered a trigger. There is also a theory (hypothesis) of a ‘deep Koebner phenomenon’ which might initiate psoriatic arthritis, although this is yet to be proven.
Getting a diagnosis of psoriatic arthritis The presence of psoriasis may provide an indication of psoriatic arthritis when someone develops joint symptoms. Psoriatic arthritis can develop in people with a lot or a little of psoriasis, and may be more common in people with nail psoriasis. As well as joint symptoms, psoriatic arthritis can lead to feeling tired. Many people become frustrated by a lack of diagnosis; psoriatic arthritis tends to have periods of improvement and worsening, which may also be attributed to mechanical joint problems and not inflammatory arthritis.
If you have the symptoms of inflammatory arthritis, such as psoriatic arthritis, your doctor will often refer you to a rheumatologist. In some cases, further tests (blood) and imagery (X-ray, ultrasound, MRI) may be sought, although this will depend on the individual circumstances and level of confidence in the initial diagnosis.
In most instances, specific treatment to the foot is necessary to some degree. Treating psoriatic arthritis in the foot will include many of the therapies used in managing arthritis elsewhere. The aim of therapy is to reduce inflammation, pain and avoid permanent disability.
Initial treatment is likely to include analgesia (pain relief), often anti-inflammatory painkillers are recommended, such as ibuprofen, or those that can be supplied Over The Counter (OTC). To treat the inflammation and swelling a prescription-only Medicine (POM) may be required and would only be available from your doctor. Treatments may include corticosteroid injections to the worst involved areas (painful, but effective for up to 6 months), oral (tablet) corticosteroids, anti-inflammatory gels and diseasemodifying drugs such as methotrexate. Sometimes, in large joints, a procedure called arthrocentesis is carried out. This involves drawing out (aspirating) the fluid for investigation for infection and the diagnosis of inflammatory conditions. The treatments listed above may only be prescribed if you have seen a rheumatologist. See Treatments for psoriatic arthritis.
Orthopaedic surgery to correct deformed joints is only justified in the presence of long-standing deformity where pain is preventing adequate mobility and all alternative medical treatments have failed. The advancement of newer techniques in recent years has seen better results in small joint replacement, but such procedures still need careful consideration and discussion with advice from an appropriate surgeon.
It is always advisable to rest severely inflamed joints, but physiotherapy and exercise can help to maintain mobility of your joints so they are less likely to become stiff and seize up. See Physiotherapy and exercise: Psoriatic arthritis
Anti-inflammatory drugs can help to reduce pain, swelling and stiffness. Unfortunately, however, they can make skin symptoms worse in some people. Steroid injections to joints may give relief. Diseasemodifying drugs such as methotrexate can dampen down both skin and joint symptoms, as can targeted biologic agents.
In some cases, surgery to remove a thickened synovial membrane (synovectomy), realign a joint (osteotomy) or to fuse a joint (arthrodesis) may stop pain which results from movement.
Sometimes it is possible to remove the painful end of a bone (excision arthroplasty).
Remember: All treatments may have unwanted side effects or require special precautions (eg during pregnancy). Always make sure you have all the information before embarking on any course of therapy; this includes reading the patient information leaflets (PILs) provided with your medicines.
If you develop problems with your foot, such as sores, rashes, nail deformities or painful swollen joints, do remember that they may not be caused by psoriasis or psoriatic arthritis.
The most important action is to seek advice and help when you notice any changes in your foot, whatever they may be. You can talk to your GP or local pharmacist for advice. Some problems can be resolved simply. For issues that are more persistent you may be referred to a specialist, such as a dermatologist, rheumatologist, physiotherapist, surgeon or chiropodist/podiatrist.
For general foot care, personal hygiene is important, particularly in avoiding fungal and viral infections. Change shoes and socks regularly, avoid shoes which are ill-fitting or cause bad posture. If you are overweight, losing weight could relieve the pressure on your joints and improve your walking gait.
If you are diagnosed with psoriasis, develop a treatment regime that works for you; often, applying treatment after a bath or shower, along with the use of an emollient, can make the process easier.

If you have nail involvement, keep nails trimmed and clean. If they are thick, try trimming them after soaking them in a bath or shower, as this makes them softer and easier to cut. Alternatively, seek an appointment with a chiropodist, which is often available via the NHS.
If you have psoriatic arthritis, it is important to rest inflamed joints. Sourcing footwear that supports the foot and helps to reduce the pressure on the inflamed areas can help, as can inner soles and orthotic supports. Once again, a chiropodist is best placed to advise you.
This article is adapted from The psoriatic foot leaflet.
Download our Psoriatic foot leaflet as a PDF
Always consult your doctor or healthcare provider.